How can we help you, Buffalo?
Recognized for Excellence
Time and Time Again!
Great Lakes Medical Imaging has been awarded the American College of Radiology® Diagnostic Imaging Center of Excellence. This honor is above and beyond the gold seal standard of ACR accreditation. We are proud to hold this honor as our commitment to excellence.

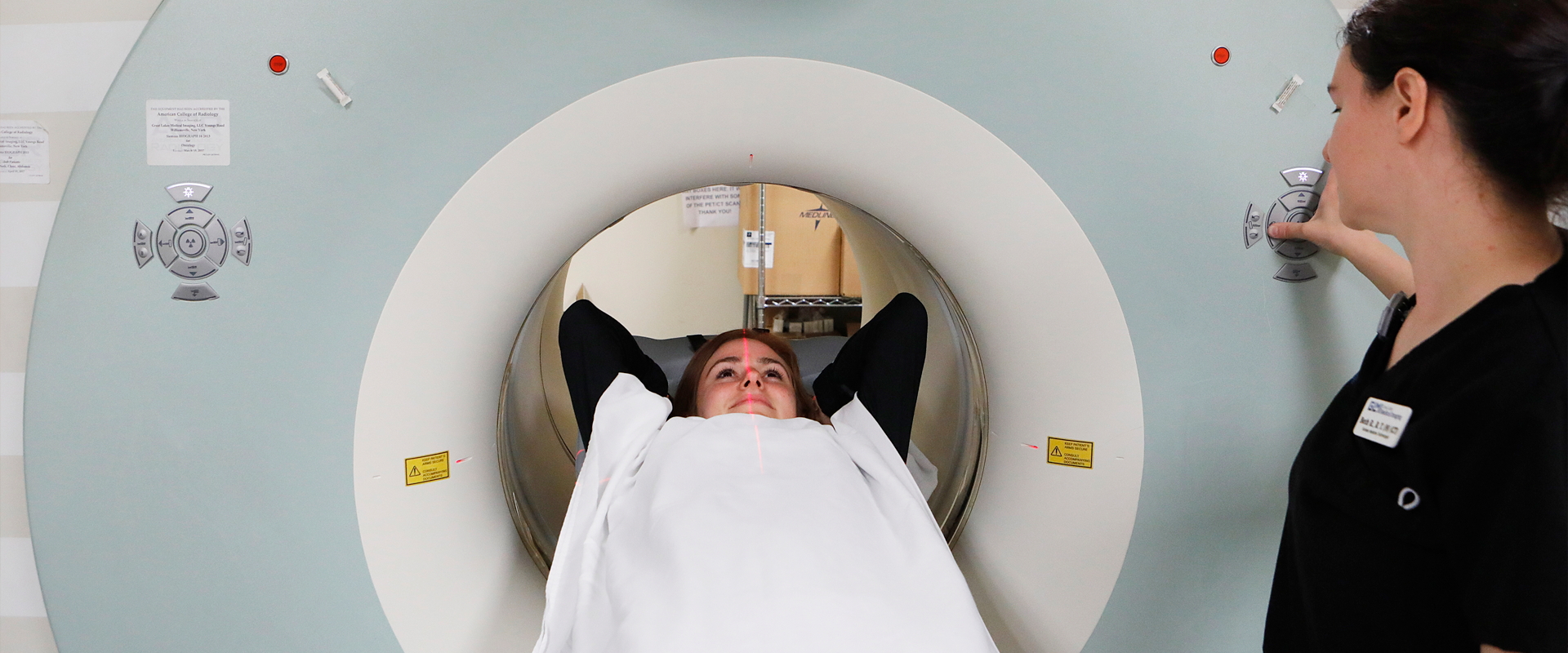
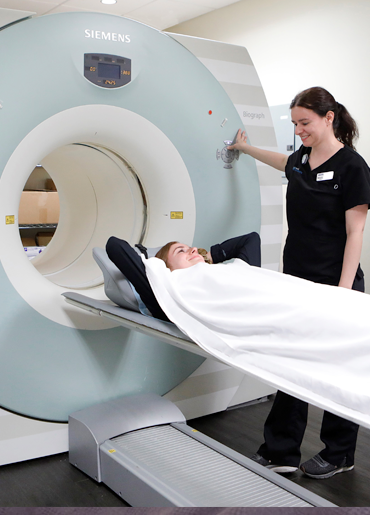
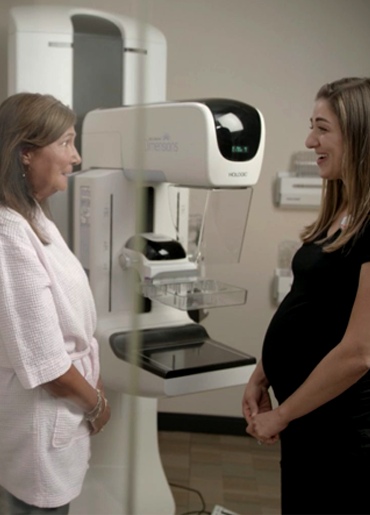
Great Lakes Medical Imaging (GLMI) is dedicated to providing the highest quality imaging for you and your family.
Our medical expertise and technology allow us to offer accurate, timely results in a comfortable setting.
These are just a few of the reasons why we are trusted by patients and physicians throughout Western New York – and why the Buffalo Bills and Buffalo Sabres both selected GLMI as their provider for imaging services.
Imaging provider partner for the
Buffalo Bills

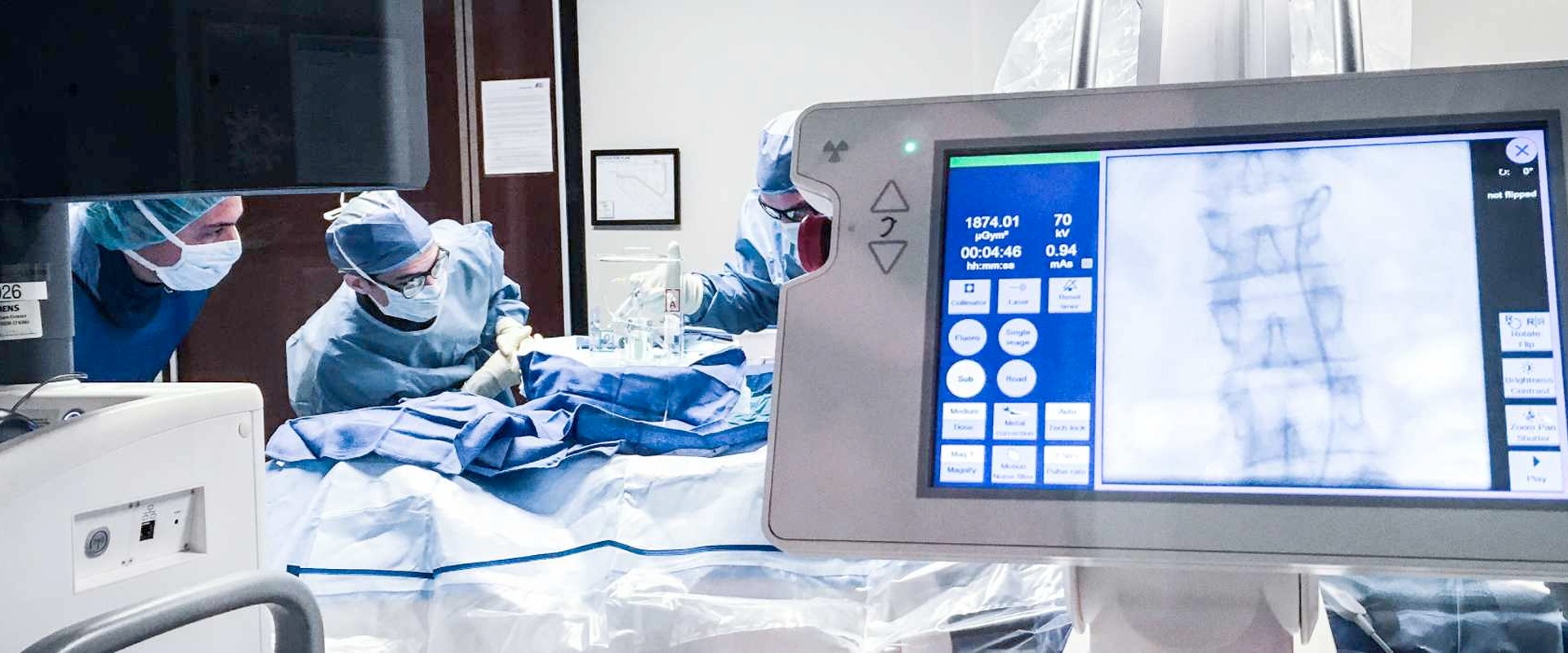
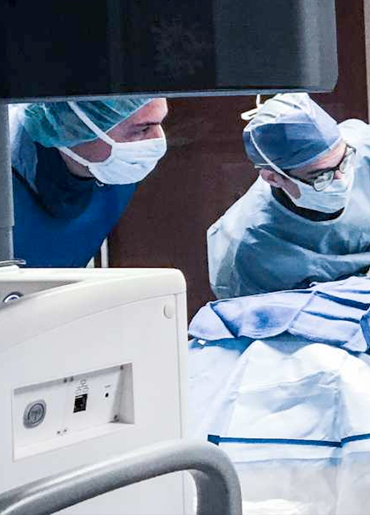
We are proud to partner with the Buffalo Bills to provide imaging services to the team. Our expertise in musculoskeletal imaging helps diagnose complex athletic injuries.
Jacobs School of Medicine and Biomedical Science

Great Lakes Medical Imaging has partnered with the University at Buffalo Jacobs School of Medicine and Biomedical Sciences as UB Radiology to direct the training of radiology residents at our affiliate hospitals and outpatient offices.
Introducing our new
Patient Portal!
We are so proud to give our customers a
new easy client portal to use! Login today!

Need help? Have questions? ! Contact Us today!
See What Your Neighbors Are Saying About Us!
What's Going on at Great Lakes?
Stay up to date with all that we have going on here at Great Lakes Medical Imaging!
See more of Great Lakes Medical Imaging
Did you know we're on instagram? Connect with us @glmirad!
We offer our patients convenient, accessible care with multiple locations throughout Western New York.
Cheektowaga
Niagara
Orchard Park - Sterling Park
Orchard Park- Big Tree
Williamsville




 Brand New State of The Art Center!
Brand New State of The Art Center!